Abstract
Corticosteroids (CS) represent first-line treatment for gastrointestinal graft vs host disease (GI GVHD), and CS failure is associated with severe morbidity and mortality. While the immune system is the intended target of CS treatment, the glucocorticoid receptor (GR) is widely expressed, and there is limited understanding of the direct effects of CS on intestinal epithelium following immune-mediated damage.
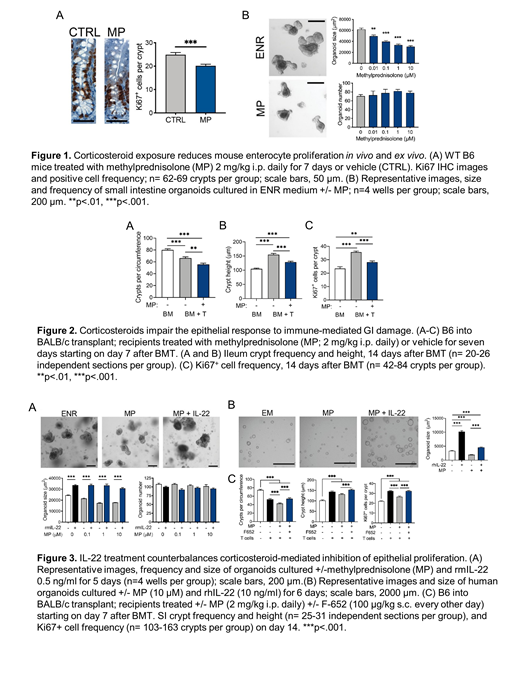
We thus investigated how CS treatment could impact intestinal homeostasis and regeneration following experimental bone marrow transplantation (BMT). In healthy C57BL/6 (B6) mice, in vivo administration of clinically relevant CS doses reduced Ki67 + epithelial proliferation in the ileum (p<0.001; Fig. 1A) without inducing crypt loss or overt pathology. Given the numerous potential effects of systemic administration, we next utilized ex vivo small intestine (SI) organoid cultures to explore direct effects of CS on murine and human epithelium. Assessing a variety of clinically relevant CS agents, we found that methylprednisolone (MP), dexamethasone, and budesonide all decreased murine organoid size without affecting organoid number (p<0.05; only MP shown; Fig. 1B). We also identified that GR-deficient (Nr3c1 -/-) organoids were significantly resistant to growth inhibition by MP (p<0.05), indicating a direct GR-mediated effect of CS on intestinal epithelium leading to reduced growth. Furthermore, MP treatment significantly decreased the size of human organoids generated from primary duodenal tissue without affecting organoid numbers (p<0.001). Organoid culture models were thus highly consistent with the findings from in vivo CS treatment.
We next investigated CS effects on epithelial cells during immune-mediated damage. Pre-treatment of mice with 2 mg/kg MP x 7 days in vivo prior to crypt harvest and organoid culture increased organoid sensitivity to T-cell-mediating killing ex vivo (p<0.05). Additionally, modeling steroid-refractory disease, GR-deficient (Nr3c1 -/-) T cells mediated greater killing of SI organoids if co-cultures were performed in the presence of MP (p<0.01). We next investigated CS-mediated effects on epithelial damage in vivo, treating with MP x 7 days starting on day 7 after MHC-mismatched BMT, once GVHD had already been established. Vehicle-treated mice demonstrated GVHD-associated T cell activation, lymphocytic tissue infiltration, and ileal crypt loss compared to BM only controls, as well as increased height and Ki67 + cell frequency in residual crypts reflecting damage-induced regeneration (p<0.001, Fig. 2A-C). Modeling steroid-refractory disease, systemic CS treatment failed to reduce T cell activation or lymphocytic infiltration. However, MP treatment appeared to attenuate regeneration and worsen intestinal pathology, as evidenced by exacerbated crypt loss in association with reduced crypt height and Ki67 + cell frequency (p<0.01; Fig. 2A-C).
Despite potential harmful side effects, CS are frequently necessary for treatment of clinical GVHD. We hypothesized that CS-mediated epithelial suppression could be mitigated by concurrent administration of agents capable of inducing tissue regeneration. Interleukin-(IL)-22 has been shown to promote epithelial proliferation and recovery following GI damage. We thus investigated whether IL-22 treatment could counterbalance CS-induced impairment of epithelial recovery in GVHD. Indeed, addition of IL-22 to MP-treated organoids promoted organoid growth without inducing toxicity/organoid loss in both murine and human SI organoid cultures (p<0.001; Fig. 3A and B). Moreover, IL-22 administration in vivo with F-652, a clinical grade recombinant human IL-22 dimer, reversed MP-mediated crypt loss and reduction of crypt height and Ki67 + cell frequency in mice with GVHD (p<0.001; Fig. 3C).
In summary, these findings indicate that CS treatment can suppress epithelial proliferation in the intestines and exacerbate GI damage if it fails to control the pathologic immune response. However, deleterious CS side effects can be counterbalanced by promotion of epithelial regeneration, providing rationale for combining immunosuppression with tissue-supporting therapeutics such as IL-22 to optimize intestinal recovery in GVHD.
Blazar: Magenta Therapeutics: Membership on an entity's Board of Directors or advisory committees; BlueRock Therapeutics: Membership on an entity's Board of Directors or advisory committees, Research Funding; Rheos Medicines: Research Funding; Equilibre Pharmaceuticals Corp: Research Funding; Carisma Therapeutics, Inc: Research Funding; Tmunity Therapeutics: Other: Co-founder. Hanash: Evive Biotech: Ended employment in the past 24 months.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal